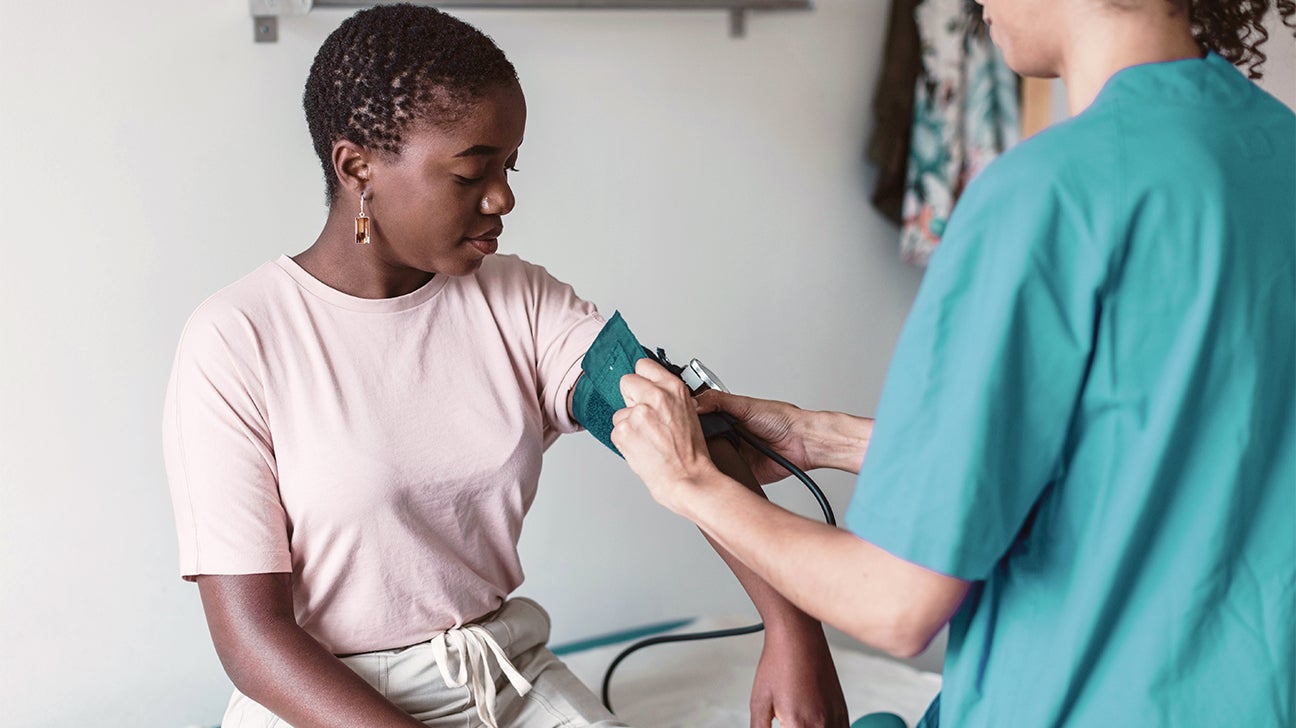
Elevated blood pressure, known as hypertension, continues to be a widespread and difficult health issue globally. Impacting numerous people around the world, it significantly contributes to heart disease, strokes, kidney failure, and other severe health issues. Although many individuals manage to control their blood pressure through typical medications and changes in lifestyle, there is a notable group that still encounters high levels even after various treatments. This type of hypertension, commonly called treatment-resistant or difficult-to-manage high blood pressure, has led researchers and medical professionals to investigate new treatment strategies.
Traditionally, hypertension management involves a combination of lifestyle interventions—such as dietary modifications, increased physical activity, stress reduction, and limiting alcohol intake—alongside pharmacological therapy. Standard medications include diuretics, angiotensin-converting enzyme (ACE) inhibitors, angiotensin receptor blockers (ARBs), calcium channel blockers, and beta-blockers. For most patients, these strategies successfully reduce blood pressure to safe levels. However, studies indicate that up to 15% of individuals with hypertension continue to exhibit high blood pressure despite adherence to multiple medications, highlighting a critical need for alternative approaches.
Researchers have increasingly focused on understanding the underlying mechanisms that contribute to treatment-resistant hypertension. In many cases, the condition is linked to a combination of genetic predisposition, overactive sympathetic nervous system activity, kidney dysfunction, hormonal imbalances, and structural changes in blood vessels. Identifying these contributing factors is essential, as it can guide the development of targeted therapies that go beyond conventional medications.
Recent advances in medical research suggest several promising strategies that may revolutionize the management of resistant hypertension. One such approach involves neuromodulation therapies, which target the nerves responsible for regulating blood pressure. For example, renal denervation—a procedure that disrupts overactive nerves in the kidneys—has shown potential in lowering blood pressure in patients who do not respond to standard treatments. Early clinical trials indicate that this minimally invasive intervention can lead to sustained reductions in systolic and diastolic blood pressure, offering hope for patients with limited options.
Another promising direction is the creation of innovative drugs that focus on unexplored pathways related to blood pressure management. These therapies aim to address the fundamental physiological processes instead of merely inhibiting the actions of existing hormones or compounds. For example, medications that target the endothelin pathway, a key regulator of blood vessel tone, or the mineralocorticoid receptor, impacting sodium and fluid balance, are currently being researched. These treatments have the potential to offer more accurate and efficient blood pressure regulation for individuals with difficult-to-treat hypertension.
Lifestyle adjustments remain vital, even for treatment-resistant hypertension scenarios. Studies highlight the need for personalized methods that take into account individual risk factors, lifestyles, and health histories. Nutritional plans, including the DASH diet—focused on consuming fruits, vegetables, whole grains, and low-fat dairy while reducing sodium—continue to show great effectiveness. Moreover, consistent physical exercise, stress reduction practices such as mindfulness and meditation, and sustaining a healthy weight can enhance the effects of pharmacological or procedural treatments, improving overall therapeutic results.
The use of continuous monitoring technologies has also emerged as a key component in managing hard-to-control hypertension. Wearable devices, home blood pressure monitors, and telehealth platforms allow for real-time tracking of blood pressure trends, medication adherence, and lifestyle behaviors. These tools enable healthcare providers to identify patterns, adjust treatment plans promptly, and provide personalized guidance. The integration of digital health solutions into hypertension management has the potential to improve patient engagement, adherence, and clinical outcomes, particularly for those with resistant forms of the condition.
Patient education remains another critical factor in addressing treatment-resistant hypertension. Individuals who understand the nature of their condition, recognize the importance of consistent medication use, and are aware of the potential impact of diet and lifestyle choices are more likely to achieve better blood pressure control. Healthcare teams are increasingly emphasizing comprehensive education programs that provide practical strategies, motivational support, and resources to empower patients in managing their condition effectively.
Scientists are investigating how genetics contributes to hypertension that doesn’t respond to treatment. Progress in genomic science has shown that specific genetic differences might affect individual reactions to drugs and environmental influences. Recognizing these genetic aspects could lead to tailored medical treatments, enabling healthcare providers to choose the most suitable therapies for each individual. This degree of accuracy has the potential to greatly enhance results and minimize the trial-and-error method often linked with controlling stubborn hypertension.
Clinical studies are presently being conducted to assess the safety and effectiveness of these new treatments. Initial outcomes appear encouraging, suggesting that a mix of procedural techniques, specific pharmaceuticals, lifestyle improvements, and digital tracking can significantly lower blood pressure in patients who previously faced limited options. As these results gain confirmation in larger, extended-duration investigations, medical professionals may shortly have a stronger set of tools for tackling one of the most difficult types of hypertension.
It is also important to recognize the broader public health implications of treatment-resistant high blood pressure. Uncontrolled hypertension contributes to significant morbidity and mortality, placing a substantial burden on healthcare systems and economies. By developing more effective management strategies, there is potential not only to improve individual patient outcomes but also to reduce the incidence of cardiovascular events, kidney disease, and associated healthcare costs.
Taking preemptive actions continues to be fundamental in controlling hypertension. Promoting regular blood pressure evaluations, endorsing diets that benefit heart health, encouraging consistent exercise, and tackling social health factors can assist in lowering the occurrence of resistant hypertension among people. Recognizing individuals at high risk early on enables prompt measures, which can avoid the condition from advancing to a state resistant to treatment.
Healthcare professionals emphasize that managing treatment-resistant hypertension requires a collaborative, multidisciplinary approach. Cardiologists, nephrologists, primary care physicians, dietitians, mental health professionals, and patient educators all play a role in developing comprehensive care plans. By integrating medical, behavioral, and technological strategies, healthcare teams can address the complex factors that contribute to persistent high blood pressure.
Although hypertension that is resistant to treatment poses a significant obstacle, novel strategies are being developed that provide optimism for patients who have had difficulty managing their blood pressure using traditional techniques. Advances in neuromodulation, precise pharmacology, digital health solutions, genetic insights, and lifestyle improvements are revolutionizing how healthcare professionals tackle this issue. Ongoing research, patient involvement, and cooperation among medical practitioners are ushering in a new phase of managing challenging high blood pressure, promising better results, fewer complications, and enhanced quality of life for millions of people across the globe.